MAKE PROTECTION
YOUR SUPERPOWER
JARDIANCE® protects by reducing risk for
adult patients with CKD*1,2, HF†3,4 and T2D+eCVD.‡5

DID YOU KNOW THAT CKD ACTS AS A RISK MULTIPLIER?6,7
Cardio, renal, and metabolic diseases are
interconnected!8


HELP PROTECT YOUR PATIENTS WITH JARDIANCE®
Early intervention is the best way to help protect patients from these interrelated conditions6,9-12
JARDIANCE® offers a range of benefits for your
patients with T2D+CVD1
IN ADULT PATIENTS WITH T2D+CVD§
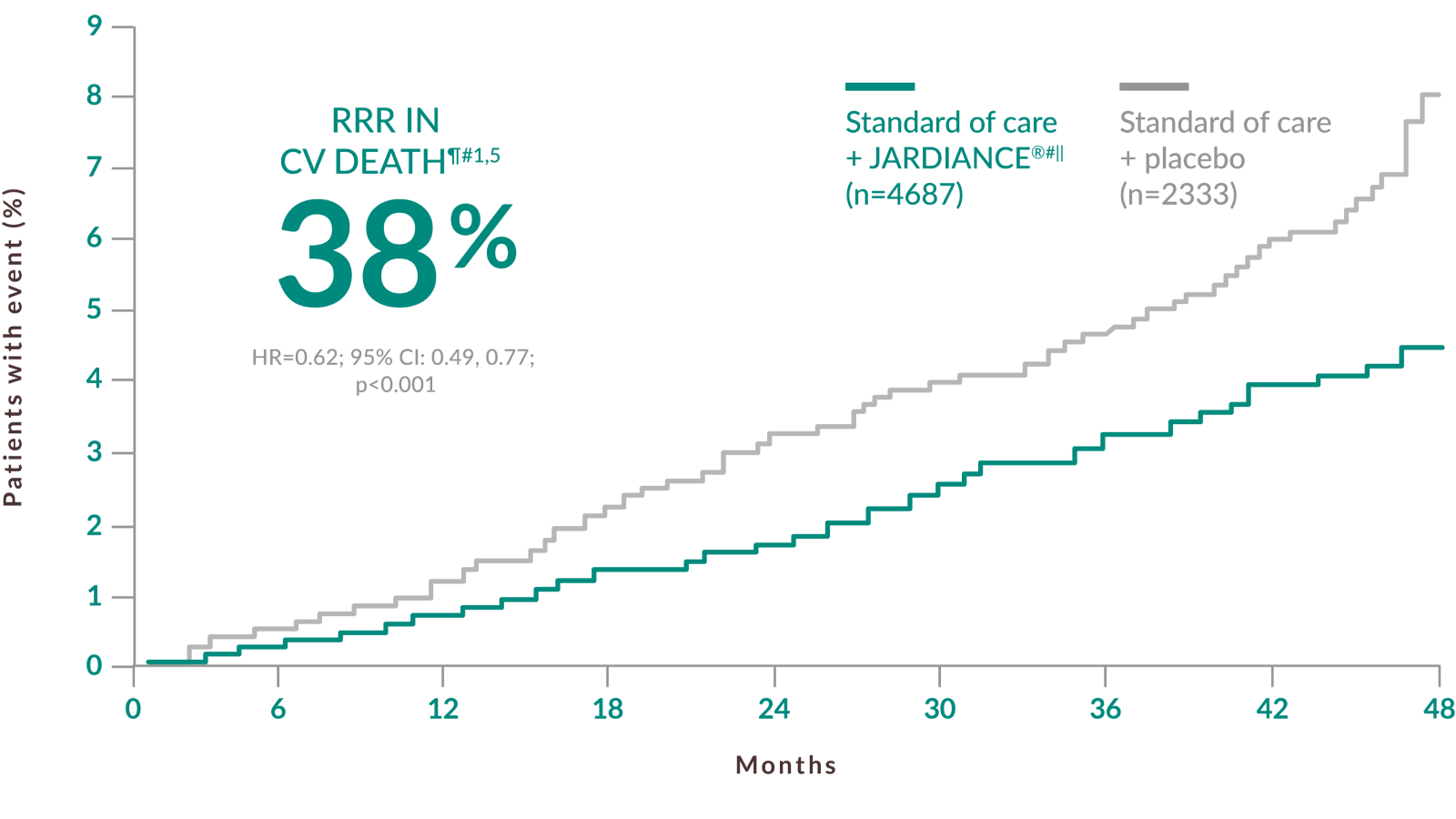
38 % RRR IN CV DEATH‡1,5
IN ADULT PATIENTS WITH T2D + CVD§
4.5 Years Life Extension vs. Placebo

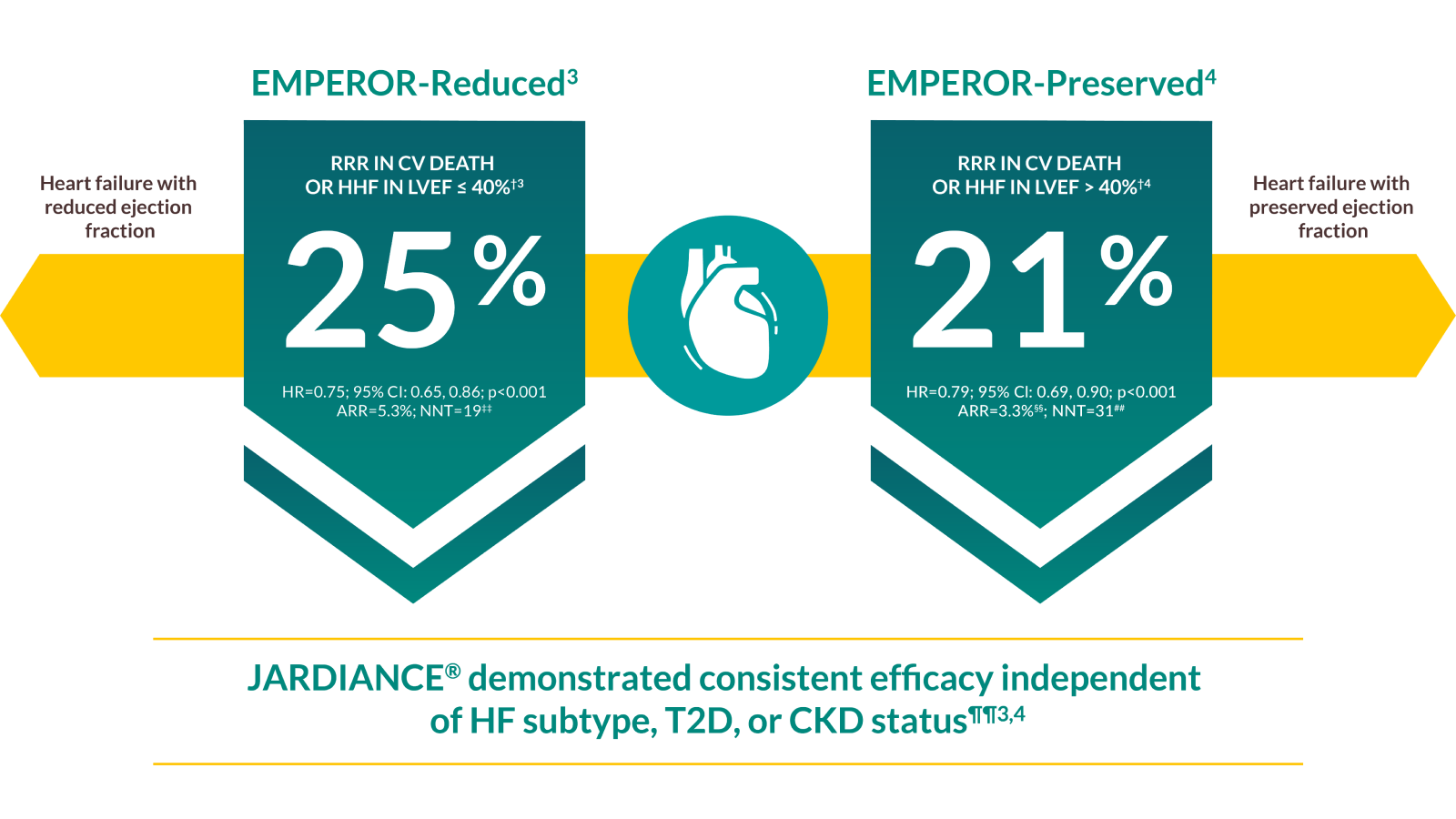
IN ADULT PATIENTS WITH CHRONIC HEART FAILURE††
HF Benefits irrespective of T2D1,3,4
Related Content

GUIDELINE RECOMMENDATIONS

DOSING RECOMMENDATIONS

SAFETY & TOLERABILITY PROFILE
Indication & Footnotes
JARDIANCE® is indicated for the treatment of adults and children aged 10 years and above for the treatment of insufficiently controlled type 2 diabetes mellitus as an adjunct to diet and exercise
as monotherapy when metformin is considered inappropriate due to intolerance
in addition to other medicinal products for the treatment of diabetes
JARDIANCE® is indicated in adults for the treatment of symptomatic chronic heart failure.
JARDIANCE® is indicated in adults for the treatment of chronic kidney disease.
-
*
In the EMPA-KIDNEY trial, a randomised, parallel-group, double-blind, placebo-controlled study of 6609 patients with CKD, the efficacy and safety profile of JARDIANCE® 10 mg (n=3304) was evaluated vs placebo (n=3305). The primary endpoint in the EMPA-KIDNEY trial was a composite of CV death or progression of kidney disease defined as end-stage kidney disease (the initiation of maintenance dialysis or receipt of a kidney transplant), a sustained decrease in the eGFR to <10 ml/min/1.73 m2, a sustained decrease in eGFR of ≥40% from baseline, or death from renal causes. Patients treated with JARDIANCE® experienced a 28% RRR in this endpoint (HR=0.72; 95% CI: 0.64, 0.82; p<0.001).2
-
†
In the EMPEROR-Reduced trial, a randomised, double-blind, parallel-group, placebo-controlled study of 3730 patients with HFrEF, the efficacy and safety profile of JARDIANCE® 10 mg (n=1863) was evaluated vs placebo (n=1867). Patients were adults with chronic heart failure (NYHA class II, III, or IV) and reduced ejection fraction (LVEF ≤ 40%). The primary endpoint in the EMPEROR-Reduced trial was a composite of CV death or HHF, analysed as time to the first event. Patients treated with JARDIANCE® experienced a 25% RRR in this endpoint (HR=0.75; 95% CI: 0.65, 0.86; p<0.001). In the EMPEROR-Preserved trial, a randomised, double-blind, parallel-group, placebo-controlled study of 5988 patients with HFpEF, the efficacy and safety profile of JARDIANCE® 10 mg (n=2997) was evaluated vs placebo (n=2991). Patients were adults with chronic heart failure (NYHA class II, III, or IV) and preserved ejection fraction (LVEF > 40%). The primary endpoint in the EMPEROR-Preserved trial was a composite of CV death or HHF, analysed as time to the first event. Patients treated with JARDIANCE® experienced a 21% RRR in this endpoint (HR=0.79; 95% CI: 0.69, 0.90; p<0.001).3,4
-
‡
The primary composite outcome in the EMPA-REG OUTCOME® trial was 3-point MACE, composed of death from CV causes, nonfatal MI, or nonfatal stroke, as analyzed in the pooled JARDIANCE® group vs the placebo group. Patients were adults with insufficiently controlled T2D and CAD, PAD, or a history of MI or stroke. The 14% RRR in 3-point MACE (HR=0.86; 95% CI: 0.74, 0.99; p<0.001 for noninferiority; p=0.04 for superiority) was driven by a reduction in the risk of CV death (HR=0.62; 95% CI: 0.49, 0.77).5
-
§
Adult patients with insufficiently controlled T2D and CAD, PAD, or a history of MI or stroke.1,5
-
¶
CV death was part of the composite primary endpoint, 3-point MACE, in the EMPA-REG OUTCOME® trial (HR=0.86; 95% CI: 0.74, 0.99; p<0.001 for noninferiority; p=0.04 for superiority) and 38% RRR in CV death was achieved in the overall EMPA-REG OUTCOME® population for the duration of the trial (HR=0.62; 95% CI: 0.49, 0.77; p<0.001).1,5
-
#
Pooled data from 10-mg and 25-mg doses of JARDIANCE®; both doses showed a comparable reduction in the risk of CV death.1,5
-
||
Standard of care included CV medications and glucose-lowering agents given at the discretion of healthcare providers and according to recommendations of local guidelines.1,5
-
**
According to nonparametric age-based Kaplan-Meier estimates of the survival curve, which were based on actuarial estimates of the age-specific probabilities of death for the pooled JARDIANCE® group and the placebo group in the EMPA-REG OUTCOME® trial. At 45 years of age, the estimated mean survival was 32.1 years in the JARDIANCE® group vs 27.6 years in the placebo group (difference, 4.5 years; 95% CI: 1.3, 7.8; p=0.007).13
-
††
Adult patients with chronic heart failure (NYHA class II, III, or IV) and reduced ejection fraction (LVEF ≤ 40%).3 Adult patients with chronic heart failure (NYHA class II, III, or IV) and preserved ejection fraction (LVEF > 40%).4
-
‡‡
ARR calculation: JARDIANCE® number of patients with events 361/total number of patients 1863=19.4%; placebo number of patients with events 462/total number of patients 1867=24.7%; 24.7%–19.4%=5.3%.3
-
§§
ARR calculation: JARDIANCE® number of patients with events 415/total number of patients 2997=13.8%; placebo number of patients with events 511/total number of patients 2991=17.1%; 17.1%–13.8%=3.3%.4
-
##
ARR was estimated as the absolute difference in the proportion of events by treatment arm. NNT=1/ARR.4
-
¶¶
Results of prespecified subgroup analyses. EMPEROR-Reduced: Diabetes at baseline (HR=0.72; 95% CI: 0.60, 0.87); no diabetes at baseline (HR=0.78; 95% CI: 0.64, 0.97). eGFR (CKD-EPI) ≥ 60 mL/min/1.73 m2 at baseline (HR=0.67; 95% CI: 0.55, 0.83); eGFR (CKD-EPI) < 60 mL/min/1.73 m2 at baseline (HR=0.83; 95% CI: 0.69, 1.00).3 EMPEROR-Preserved: Diabetes at baseline (HR=0.79; 95% CI: 0.67, 0.94); no diabetes at baseline (HR=0.78; 95% CI: 0.64, 0.95). eGFR (CKD-EPI) ≥ 60 mL/min/1.73 m2 at baseline (HR=0.81; 95% CI: 0.65, 1.00); eGFR (CKD-EPI) < 60 mL/min/1.73 m2 at baseline (HR=0.78; 95% CI: 0.66, 0.91).4
ARR=absolute risk reduction; CAD=coronary artery disease; CI=confidence interval; CKD=chronic kidney disease; CKD-EPI=Chronic Kidney Disease Epidemiology Collaboration; CV=cardiovascular; CVD=cardiovascular disease; eGFR=estimated glomerular filtration rate; HF=heart failure; HFpEF=heart failure with preserved ejection fraction; HFrEF=heart failure with reduced ejection fraction; HR=hazard ratio; LVEF=left ventricular ejection fraction; MACE=major adverse cardiovascular events; MI=myocardial infarction; NNT=number needed to treat; NYHA=New York Heart Association; PAD=peripheral artery disease; RRR=relative risk reduction; T2D=type 2 diabetes.
References
-
JARDIANCE® [summary of product characteristics]. Ingelheim am Rhein, Germany; Boehringer Ingelheim International GmbH.
-
Herrington WG, Staplin N, Wanner C, et al. EMPA-KIDNEY Collaborative Group. Empagliflozin in patients with chronic kidney disease. N Engl J Med. 2023;388(2):117-127. (EMPA-KIDNEY results and the publication’s Supplementary Appendix.)
-
Packer M, Anker SD, Butler J, et al; EMPEROR-Reduced Trial Investigators Cardiovascular and renal outcomes with empagliflozin in heart failure. N Engl J Med. 2020;383(15):1413-1424. (EMPEROR-Reduced results and the publication’s Supplementary Appendix.)
-
Anker SD, Butler J, Filippatos G, et al; EMPEROR-Preserved Trial Investigators. Empagliflozin in heart failure with a preserved ejection fraction. N Engl J Med. 2021;385(16):1451-1461. (EMPEROR-Preserved results and the publication’s Supplementary Appendix.)
-
Zinman B, Wanner C, Lachin JM, et al; EMPA-REG OUTCOME Investigators. Empagliflozin, cardiovascular outcomes, and mortality in type 2 diabetes. N Engl J Med. 2015;373(22):2117-2128. (EMPA-REG OUTCOME® results and the publication’s Supplementary Appendix.)
-
GBD Chronic Kidney Disease Collaboration. Global, regional, and national burden of chronic kidney disease, 1990-2017: a systematic analysis for the Global Burden of Disease Study 2017. Lancet. 2020;395(10225):709-733.
-
Jankowski J, Floege J, Fliser D, Böhm N, Marx N. Cardiovascular disease in chronic kidney disease: pathophysiological insights and therapeutic options. Circulation. 2021;143(11):1157-1172.
-
Kalra S, Aydin H, Sahay M, et al. Cardiorenal syndrome in type 2 diabetes mellitus—rational use of sodium-glucose cotransporter-2 inhibitors. Eur Endocrinol. 2020;16(2):113-121.
-
McDonagh TA, Metra M, Adamo M, et al; ESC Scientific Document Group. 2021 ESC Guidelines for the diagnosis and treatment of acute and chronic heart failure. Eur Heart J. 2021;42(36):3599-3726.
-
Davies MJ, Aroda VR, Collins BS, et al. Management of hyperglycemia in type 2 diabetes, 2022: a consensus report by the American Diabetes Association (ADA) and the European Association for the Study of Diabetes (EASD). Diabetes Care. 2022;45(11):2753-2786.
-
Heidenreich PA, Bozkurt B, Aguilar D, et al. 2022 AHA/ACC/HFSA Guideline for the Management of Heart Failure: a report of the American College of Cardiology/American Heart Association Joint Committee on Clinical Practice Guidelines. J Am Acad Cardiol. 2022;79(17):e263-e421.
-
Kidney Disease: Improving Global Outcomes (KDIGO) CKD Work Group. KDIGO 2012 Clinical Practice Guideline for the Evaluation and Management of Chronic Kidney Disease. Kidney Int. 2013;3(1):1-150.
-
Claggett B, Lachin JM, Hantel S, et al. Long-term benefit of empagliflozin on life expectancy in patients with type 2 diabetes mellitus and established cardiovascular disease: survival estimates from the EMPA-REG OUTCOME trial. Circulation. 2018;138(15):1599-1601.